As it turns out, the most accurate and non-invasive way to test for a hole in the heart is not to look at the heart at all, but to look at your brain! My sonographer, Dan Traves and I have been pioneering this method in Australia for many years – thus Heartbrain Private Clinic’s neuro-cardiac solutions clinic was borne. But let’s start at the beginning…
What are the symptoms?
Some people can have a PFO their entire life and never experience any symptoms; while for others it can cause a myriad of problems – however they are not always easy to recognise.
Some examples of symptoms or medical conditions that PFO can be confused with are:
• Stroke, mini-stroke, severe migraine with aura, exertional headache, ‘brain fog’
• Chronic fatigue syndrome
• Asthma, exertional breathlessness, difficulty achieving fitness, sleep apnoea
• Altitude sickness, decompression illness
What can I do if I’m experiencing symptoms?
Through my medical experience and research at the PFO Research Foundation, I have uncovered many conditions and diseases that could be the result of, or highly affected by, a PFO – however, it may take some time before these links are well known and widely accepted. Therefore it could take years before you are referred to check for a PFO.
The best way is to educate yourself and take a proactive approach to your own health care.
If you are experiencing any symptoms, visit your GP and ask for a referral to Heartbrain Private Clinic.
Although our PFO test is a simple one, we don’t just perform it on anyone. There are certain criteria you’ll need to meet before we decide if you need to be screened for a PFO.
What does the screening involve?
At Heartbrain Private Clinic, we are the first in Australia to use a non-invasive test that is safer, faster and more accurate than the accepted ‘gold standard’.
Instead of the invasive Trans-Oesophageal Echocardiogram (TOE), which requires day admission to a hospital and an ultrasound probe down the oesophagus, we first perform a Transcranial Doppler (cTCD) ultrasound with contrast.
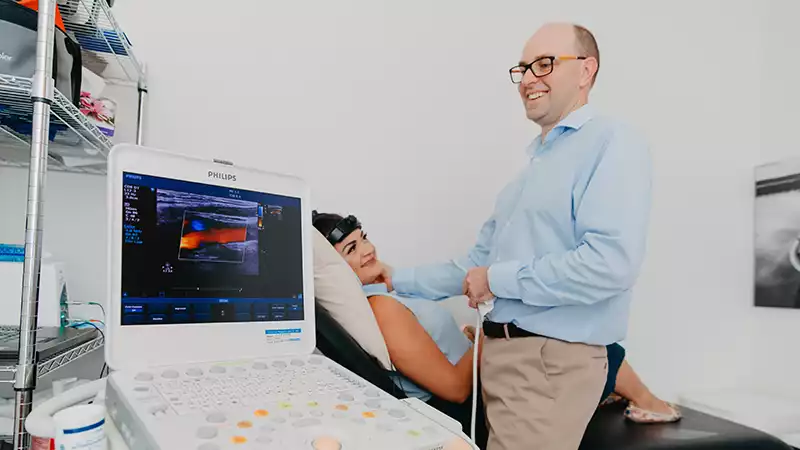
The cTCD involves a small amount of saline being injected into your blood stream while we monitor your brain activity. We are looking to see if any of the saline reaches the brain, indicating that some unfiltered blood is being pumped around your body.
The whole procedure takes around 15 minutes in our office, and you can go back to work straight away.
For more details on the cTCD, see Screening for a PFO.
If I have a PFO, what’s next?
Following the confirmation of a probable PFO using the Transcranial Doppler (cTCD) test, we may need to perform further investigations to confirm the type of hole, its location and physical characteristics.
Depending on the size and the symptoms of your PFO, I may recommend closing it. This is not always the case and depends on linking the hole size as causal to your condition. Small holes are common and may not have any role to play -the cTCD grading also gives me a ‘hole size’ estimation. If it is large, and as if you’ve come this far as to see me, the PFO must be impacting your life so it is likely I will recommend closure.
Closing the PFO
Closing the PFO involves inserting a patch device that will vary in size depending on the size of your hole. I have evolved and altered the techniques to allow for minimally-invasive PFO closure to be done in just 20 minutes with same-day discharge.
Our method involves local anaesthetic, twilight sedation (don’t worry you won’t remember a thing!) and locating the hole rapidly with a specially shaped catheter (our invention) that then allows the hole to be found in seconds and the patch to be delivered via a 2mm cut in the groin with positioning of the patch under X-Ray.
Most other centres have a procedural time of one to two hours. We are done and dusted in 20 minutes having evolved this revolutionary technique.
Patients are discharged on the same day or the following morning. A gentle walk the next day is encouraged. The only restrictions are no heavy lifting or straining for two weeks and no maximal exercise for a month.

What can I do?
We have a very structured, proven and efficient process to rapidly and accurately assess for PFO, allowing our team to deliver effective treatment strategies quickly.
If you are experiencing any or a combination of the above symptoms, or have had a cryptogenic stroke, visit your GP for a referral to Heartbrain Private Clinic.
Eligible patients may be invited to join one of our many research projects that are conducted through the PFO Research Foundation, a registered charitable organisation dedicated to advancing the science, and to educate the general public and medical community about PFO-related disease.
